New Data Show a Dip in the RN Workforce
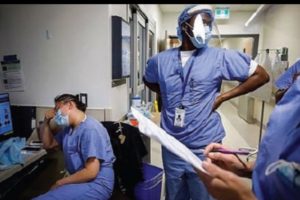 After decades of robust growth in the nursing workforce, an analysis of health care employment in 2021 found more than 100,000 fewer RNs than in 2019, a 1.8% drop in the prepandemic workforce. The greatest loss was in the hospital sector (3.9%), which was partially offset by a 1.6% growth in other RN work settings. Also notable was a 4% reduction in acute care RNs younger than age 35, compared with significantly less attrition among RNs ages 35 to 49 (0.5%) and those older than age 50 (1%).
After decades of robust growth in the nursing workforce, an analysis of health care employment in 2021 found more than 100,000 fewer RNs than in 2019, a 1.8% drop in the prepandemic workforce. The greatest loss was in the hospital sector (3.9%), which was partially offset by a 1.6% growth in other RN work settings. Also notable was a 4% reduction in acute care RNs younger than age 35, compared with significantly less attrition among RNs ages 35 to 49 (0.5%) and those older than age 50 (1%).
The analysis, published April 13 in Health Affairs Forefront, is an extension of a January Health Affairs analysis of data from the Current Population Survey. The losses in the nursing workforce contrast with more than 40 years of near continuous growth; the authors calculated 1 million RNs in 1982 compared with 3.2 million in 2020. These new data, coupled with an estimated 70,000 boomer RNs expected to retire annually by 2030, suggest the hospital workforce will be sorely stressed as experienced nurses leave the bedside.
This shouldn’t be a surprise to anyone. Nurses have been decrying hospital staffing shortages for years, which the COVID-19 pandemic only exacerbated. Inadequate personal protective equipment; overwhelming numbers of extremely ill patients; and the departure of colleagues who decided to retire, leave for higher-paying travel nurse jobs, or simply quit the profession added to stress and burnout, especially among younger nurses, according to surveys and interviews with nurse executives and leaders:
- In a May 2021 AMN Healthcare survey of 6,562 RNs who provided direct care, 63% of whom were hospital based, approximately 23% of respondents said it was “somewhat likely or extremely likely” they would leave nursing because of the pandemic. Seventy-one percent of respondents were in their current position for five years or less.
- The January 2022 Pulse on the Nation’s Nurses Survey by the American Nurses Foundation reported responses from 12,694 nurses. Two out of three nurses younger than age 35 reported feeling burned out, and 63% of all respondents said they intended to or were considering leaving their jobs, mainly because of insufficient staffing and the negative health effects of work. Other reasons given were inability to provide quality care, distrust of employer, lack of employer support, need for higher income, and poor organizational response to COVID-19.
Although such surveys have consistently underscored the stress and exhaustion experienced by nurses and other health care workers during COVID-19, it is difficult to extrapolate long-term workforce consequences. The authors of the analysis acknowledge these difficulties, particularly when it comes to disentangling all the “contributing factors” that disrupted U.S. health care delivery. Besides clinician burnout, frustration, and early retirement, they note the possible influence of “family needs such as childcare and elder care, [and] COVID-19 infection.”
This disruptive period has also yielded good news. According to a 2020 survey by the American Association of Colleges of Nursing, enrollments in four-year baccalaureate programs are on the rise, increasing 5.6% from 2019 to 2020, although applications in 2020 increased only 1.5% (increases were 4.5% and 8.5% in 2019 and 2018, respectively).
Commenting on these workforce indicators, Karen S. Hill, editor-in-chief of the Journal of Nursing Administration, told AJN, “Nurses need to know how important they are to health care and others need to recognize them and their value. This recognition must include fair, competitive salaries and benefits, as well as flexibility in scheduling and career paths. The new generation of nurses can find these characteristics in other careers, and we need to ensure they find them and more in nursing.”—Maureen Shawn Kennedy, MA, RN, FAAN
References
Auerbach DI, et al. Health Affairs Forefront 2022 Apr 13; Buerhaus PI, et al. Health Affairs 2022;41(1):79–85.
(This story originally appeared in American Journal of Nursing.)




