How can NJ cut high death rate among Black mothers in childbirth? This group has a plan
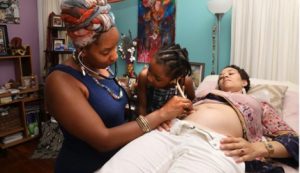 The latest plan to reduce New Jersey’s stubbornly high death rate among Black women in childbirth and the year afterward calls for diversifying the workforce that cares for pregnant and post-partum women and changing payment incentives.
The latest plan to reduce New Jersey’s stubbornly high death rate among Black women in childbirth and the year afterward calls for diversifying the workforce that cares for pregnant and post-partum women and changing payment incentives.
Unveiled Tuesday by a state health care advocacy group, the plan builds upon the successes of programs such as group prenatal visits and discussions, known as Centering Pregnancy, offered by St. Joseph’s Health in Paterson, and home visits by nurses in the first three weeks of a newborn’s life. And it supports the Nurture New Jersey awareness campaign launched by first lady Tammy Murphy to focus attention on the crisis in Black maternal mortality in New Jersey.
“We’re hoping to see a future world where patients can look to find … providers who have a similar life experience, who look like them, and speak their language,” said Linda Schwimmer, chief executive officer of the New Jersey Health Care Quality Institute, which prepared the “Maternity Action Plan.”
That workforce should include not just doctors, but an expanded number of midwives, doulas, community health workers and lactation consultants, she said. Support for new mothers should extend far beyond the walls of hospitals and doctors’ offices, and address their social, economic and mental health needs, she said.
Advocates and experts have spent years trying to address the racial gulf in childbirth experiences that causes Black women in New Jersey to die from childbirth complications at a rate seven times higher than white women, according to the Nurture New Jersey strategic plan. Black babies in New Jersey are three times more likely than white babies to die in their first year.
The death rate among Black women is higher than in any other state, according to the United Healthcare Foundation. And while the United States as a whole has the highest death rate among new mothers of any nation in the developed world, New Jersey consistently ranks among the five worst states in the country in overall maternal mortality.
That data dates mostly from 2018, so the effect of recent initiatives — including increases in state and federal funding to address the problem, and a package of 14 state laws enacted in 2019 — is not reflected. And change takes time.
“We’re in a completely different environment than we were before,” Schwimmer said, explaining why she thought the plan announced Tuesday stood a greater chance of success than previous ones.
Changes in leadership, with the Murphy administration’s intense focus on the problem, have helped, as has increased media attention and a broader understanding and acknowledgement of the role of systemic and institutional racism in health.
“More people are engaged at the community level,” she said, “and they are being listened to.” The year-long project to develop the plan was underwritten by the Robert Wood Johnson Foundation. The Quality Institute said its recommendations had been vetted by the state Department of Health.
Public reporting of data and advocacy efforts have led to a sharp drop in the rate of early elective deliveries, and have reduced the rate of cesarean sections, or surgical births, from 40% in 2016 to 26 % in 2021, based on data from the Leapfrog Group, a nonprofit watchdog group that collects survey data from hospitals.
But major changes still are needed, particularly when it comes to the way hospitals are reimbursed, she said.
For example, hospitals still receive higher payments for cesarean section births, which have a higher rate of complications for mothers and babies, than they do for vaginal births. Babies born via C-section are more likely to receive care in a neonatal intensive care unit, also reimbursed at a higher rate than a general newborn nursery.
“We would like to see care paid for in a way that rewards the highest quality maternity care,” Schwimmer said. “That is not the case today, with the exception of some pilot programs.”
Plenty of data is gathered in New Jersey about the health of mothers and babies and the performance of hospitals, but it is spread over many agencies and not easy to use.
The report recommends assembling that information in a user-friendly format that allows prospective parents to better choose their insurer, doctor or other provider and birthing location, whether hospital or childbirth center.
“We don’t want to start with a completely new slate of programs,” said Schwimmer, but to build out and support existing programs that have a positive impact on maternal and child health.
One such program at St. Joseph’s Health in Paterson, called CenteringPregnancy, received an award from the New Jersey Hospital Association on Tuesday for its work.
Pregnant women in the program participate in group discussions, led by a midwife, on topics such as nutrition, labor and delivery, breastfeeding, stress management and infant care. These “group prenatal visits” are also accompanied by one-on-one time with a health care provider. Twelve groups — six that meet in English, and six in Spanish — are currently in progress.
Since it began in February 2020, 160 women have completed the program and given birth. Those who participated had a breastfeeding rate of 90% when they left the hospital, compared to the hospital rate of 77%. Only 17% of them gave birth via C-section, compared to 30% for the hospital. And 93% attended their post-partum visits, compared to 80% for clinic patients, according to hospital data.
St. Joseph’s “cares for a very diverse and often underserved population,” said Dr. Roger Kierce, the system’s chairman of obstetrics and gynecology. “We are committed to addressing racial disparities in health care, specifically with prenatal care.”
While the goal of such programs and the recommendations of the plan announced Tuesday are to reduce racial disparities in health care, their effects ultimately will be broader, Schwimmer said.
“They address maternity care in a way that is going to improve it for everyone in the state,” she said.
(This story originally appeared in NorthJersey.com.)




