Healthcare Workers Who Wear Better Masks Get Less COVID
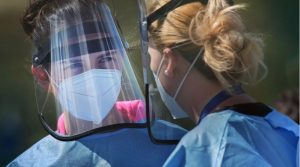 Healthcare workers had better odds of outmaneuvering SARS-CoV-2 infection while wearing a respirator mask rather than a surgical mask, an observational study showed.
Healthcare workers had better odds of outmaneuvering SARS-CoV-2 infection while wearing a respirator mask rather than a surgical mask, an observational study showed.
Among workers exposed to COVID-19 patients, those who always donned a respirator mask had a lower likelihood of infection (21% vs 35% for those that did not; OR 0.49, 95% CI 0.39-0.61), reported Philipp Kohler, MD, of Cantonal Hospital St. Gallen in Switzerland, and colleagues.
And this difference was “irrespective of cumulative exposure,” the group wrote in JAMA Network Open.
Still, Kohler said in an email conversation, the results of the study do not infer causality. “Whether healthcare workers wearing respirators also behave differently outside their working place (and thereby get less infected) remains an open question.”
Unsurprisingly, healthcare workers were more likely to test positive with greater cumulative exposure to COVID-19 patients, regardless of their mask use:
- >2 to 4 hours of exposure: 25% positive
- >8 to 16 hours: 32.9% positive
- >64 hours: 42.7% positive
But Kohler said he was really surprised to see such a “nice” dose effect for patient exposure (OR 1.20 per doubling of cumulative contact time, 95% CI 1.14-1.26). “This is something I had not expected to see.”
While working full time at least 80% of the time was also associated with an increased risk of a positive SARS-CoV-2 result (OR 1.39, 95% CI 1.10-1.77), a household contact posed the greatest risk (OR 7.79, 95% CI 5.98-10.15).
Along with always masking with a respirator, vaccination also provided protection against testing positive for SARS-CoV-2 (OR 0.55, 95% CI 0.41-0.74).
Another protective factor was being an active smoker (OR 0.68, 95% CI 0.49-0.95).
The last finding “is a bit odd,” admitted Kohler. “Smokers may have a decreased risk, but if infected … they fare worse,” he said.
Overall, this study does not provide evidence that protocols for respirator masking should be stricter, said Kohler.
“Wearing respirators is very uncomfortable if you have to do this over a long time,” he said. The risk of getting infected is probably higher when eating out in a restaurant or when having a family reunion, he added. However, “I think that particularly [healthcare workers] at risk (e.g., with immunosuppression) could benefit from wearing respirators when caring for SARS-CoV-2 patients.”
How many COVID-19 patients am I seeing? Do I have risk factors for severe disease? Am I vaccinated? “These are important questions to ask in deciding whether to use respirators or not,” Kohler added.
To compare infection risk by mask type, researchers followed 2,919 healthcare workers weekly from September 2020 to September 2021 at seven health care centers in Switzerland.
Participants (mean age 43) were screened for anti-nucleocapsid antibodies at baseline, then in January 2021 and in September 2021. Among them, 749 (26%) participants were infected with SARS-CoV-2. A positive test was also reported in 13% of participants who were not exposed to patients.
Participants reported weekly on the results of their SARS-CoV-2 nasopharyngeal swabs (PCR or rapid antigen testing), the number of exposures they had to infected patients, including mean contact duration (in a range of 1 to 60 minutes) and the type of protection used (respirator or surgical mask).
No differences in odds of SARS-CoV-2 positivity were observed for healthcare workers in the intensive care unit, or for those who visited their hospital’s canteen once or more per week (vs less often).
Disclosures
The study was supported with grants from the Swiss National Sciences Foundation, the Federal Office of Public Health, and the Health Department of the Canton of St. Gallen.
Authors reported relationships with the study funders and with Roche Diagnostics, which provided testing assays.
Primary Source
JAMA Network Open
24 Comments
(This story originally appeared in Medpage Today.)




